

Margarita Svarceva
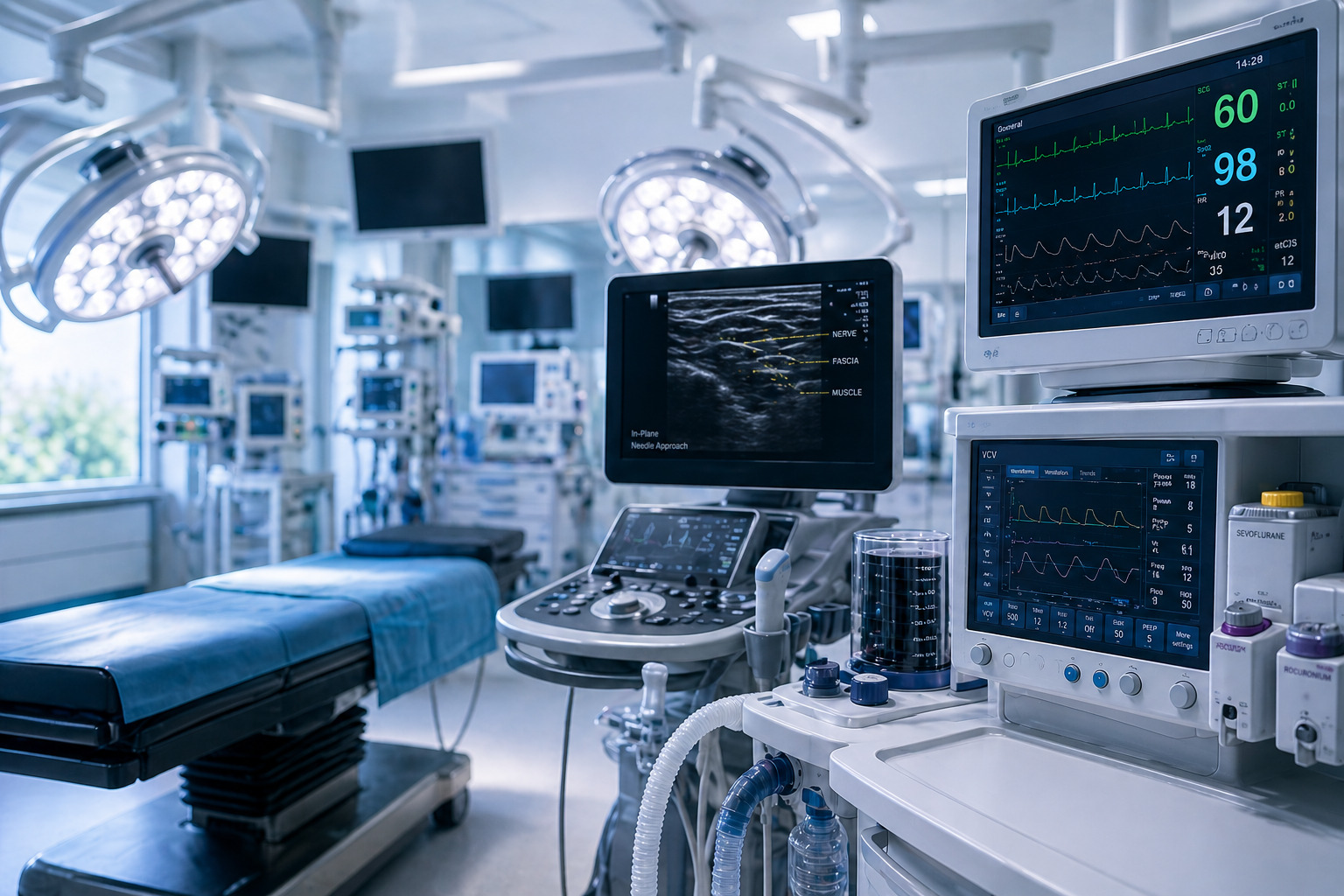
Anaesthesia is no longer judged solely on whether a patient feels pain during surgery. Increasingly, its success is defined by how quickly that patient can recover, mobilise, and return home. This shift, driven by the rise of day-case surgery and enhanced recovery pathways, has repositioned anaesthesia from a supporting function to a determinant of system performance.
This creates a clear opportunity. Approaches that can accelerate recovery while maintaining safety can unlock both better patient outcomes and more efficient use of hospital capacity. Regional anaesthesia sits at the centre of this shift.
By reducing systemic drug exposure and enabling earlier mobilisation, regional anaesthesia aligns closely with the priorities of modern surgical care. In some settings, particularly in orthopaedics or urology, it has become the dominant approach for routine procedures. In others, it remains selectively used, dependent on clinician preference and institutional practice. This uneven adoption reflects a broader reality: regional anaesthesia is not a standardised protocol, but a situational decision shaped by clinical, operational, and human factors.
The insights in this article are based on discussions Sector & Segment has had with clinicians, including surgeons and anaesthetists, across a range of specialties and countries.
Regional anaesthesia refers to techniques that numb a specific region
of the body by targeting nerves, rather than inducing full unconsciousness as in general anaesthesia. This can include spinal and epidural anaesthesia, which block sensation in the lower half of the body, as well as peripheral nerve blocks that target specific limbs or anatomical areas.
In practice, regional anaesthesia is used in multiple ways: as a standalone technique, combined with light sedation, or alongside general anaesthesia to improve postoperative pain control. Where multiple options are viable, the choice is rarely straightforward and is shaped by a combination of factors. Patient preference can play an important role, with some patients favouring being awake or lightly sedated, while others prefer to be fully unconscious during surgery. Clinical considerations are equally important: for example, spinal anaesthesia typically lasts around two hours, making expected operating time a key determinant of suitability. Workflow constraints also influence decision-making, as the time required to perform a block and allow it to take effect must fit within tightly scheduled operating lists. Finally, patient-specific factors can limit the use of regional techniques; prior spinal surgery, anatomical challenges, or cognitive impairment may make procedures such as spinal injections more difficult or inappropriate.
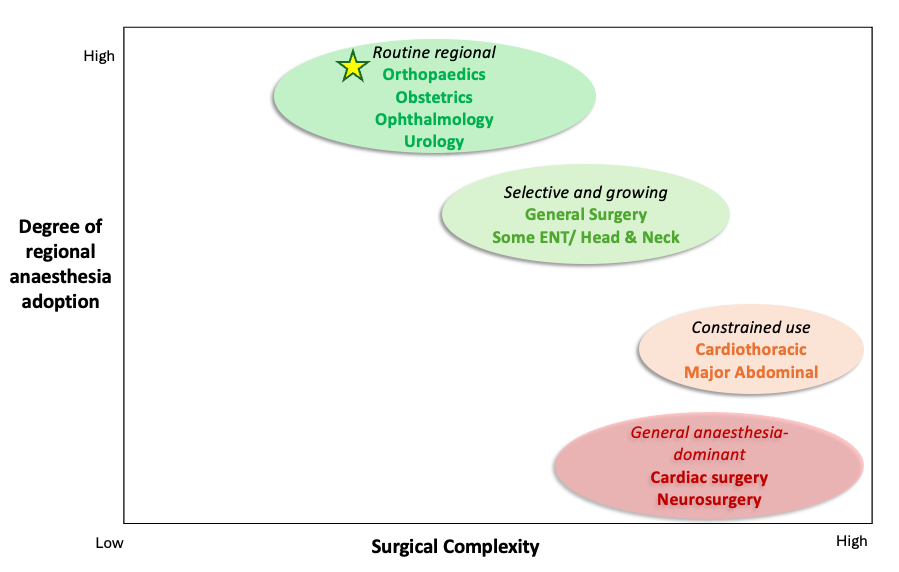
The use of regional anaesthesia varies markedly across surgical specialties, with no single pattern of adoption. In orthopaedics and obstetrics, it is widely embedded into routine practice, often forming the backbone of perioperative care, as procedures are on the shorter side and are more predictable in nature. In ophthalmology, its use is similarly high, due to the short duration and low complexity of procedures. By contrast, in specialties such as cardiothoracic surgery or neurosurgery, regional anaesthesia’s role is more limited, constrained by procedural complexity and the need for absolute physiological control during surgery.
This variation reflects fundamental differences in what each specialty prioritises. Where early mobilisation and rapid discharge are critical, regional techniques offer a clear advantage, as they preserve physiological function, reduce systemic side effects, and enable patients to regain movement sooner after surgery. Where surgical duration is long, or where airway and neurological control are paramount, general anaesthesia remains dominant, as it combines analgesia, muscle relaxation, and sedation to provide complete control over the patient throughout the procedure. As a result, regional anaesthesia is best understood not as a single one-size-fits-all approach, but as a set of specialty-specific practices.
Historically, the role of anaesthesia was straightforward: to ensure that surgery could be performed without pain. However today, that definition feels incomplete. The focus has shifted towards what happens after the procedure, how quickly the patient can stand, move, and ultimately leave the hospital. This shift is particularly visible in orthopaedics. Following procedures such as knee replacements, there is a growing expectation that patients should begin moving around on their feet on the same day. Achieving this requires not only effective pain control, but also preservation of muscle function and avoidance of systemic side effects. The combination of drugs within general anaesthesia would prevent the patient from achieving this milestone on the day of the surgery. Therefore, the choice of anaesthesia can support recovery or delay it.
"Companies need to come in and spend time in the hospital, with different departments, and talk to staff besides the anaesthetists. All departments have a different approach. It is about understanding what each person in the chain is doing, and how their role is affected – the surgeons but also the theatre staff and the operating personnel. Gone are the days when a task is only for one – we are all involved in the same patient at the same time, and that needs to be understood"
– Orthopaedic Surgeon, NHS England
Regional anaesthesia fits naturally into this new paradigm. By targeting specific nerves rather than the entire body, it avoids many of the systemic effects associated with general anaesthesia, such as nausea, respiratory suppression, and prolonged sedation. The result is a smoother and often faster recovery trajectory. Within Enhanced Recovery After Surgery (ERAS) pathways, anaesthesia is no longer an isolated decision but an integrated component of a broader recovery strategy. The growing interest in regional techniques therefore reflects a deeper alignment with how healthcare systems are being asked to operate: faster, more efficient, and more patient-centred.
While spinal and epidural anaesthesia have long been established, the most meaningful recent advances have come from the evolution of peripheral nerve blocks, particularly those designed to preserve motor function. Unlike spinal anaesthesia, which numbs a broad region of the body by acting at the level of the spinal cord, peripheral nerve blocks target specific nerves supplying a limb or surgical site, allowing for more localised and controlled effects.
“I use adductor canal blocks, a type of peripheral nerve block, for knee replacements. It’s been a game changer, incredible. The patients are pain-free for 36 hours. It’s revolutionary for the first steps of their recovery”– Orthopaedic Surgeon, NHS England
These motor-sparing approaches represent a shift in objective. Rather than simply eliminating pain, they aim to do so while maintaining the patient’s ability to move. In orthopaedic procedures, this can enable patients to walk within hours of surgery, fundamentally changing the recovery experience. At the same time, these blocks can provide extended pain relief (often lasting more than 24 hours) reducing the need for systemic post-operative painkillers and allowing patients to recover more comfortably in the immediate postoperative period.
Importantly, these techniques are not entirely new, but their adoption has accelerated significantly over the past five years. This has been driven by advances in ultrasound guidance, which have improved the precision, safety, and reproducibility of nerve targeting, as well as by a new generation of clinicians trained to use these approaches as part of standard practice. As a result, the definition of effective anaesthesia is evolving from absence of pain to facilitation of functional recovery.
Despite its advantages, regional anaesthesia has not achieved uniform adoption. The barriers are less about clinical uncertainty and more about the realities of delivering it consistently within busy, time-sensitive surgical environments.
A key challenge lies in variability. Unlike general anaesthesia, which follows a relatively standardised and predictable process, regional techniques depend heavily on clinician skill, patient anatomy, and precise execution. This introduces uncertainty at multiple stages. A block may take longer than expected to work, may not provide complete coverage, or in some cases may fail altogether, requiring conversion to general anaesthesia. Even when successful, the duration of effect can vary between patients, making it difficult to align perfectly with surgical timelines and recovery planning.
These clinical uncertainties are closely tied to workflow constraints. Performing a regional block requires preparation, equipment, and often a period of waiting for the anaesthetic to take effect before surgery can begin. In tightly scheduled operating lists, this can disrupt flow and create delays, particularly if timing is unpredictable. At the same time, regional anaesthesia is not suitable for all patients. Anatomical challenges, prior surgery, or inability to remain still can limit its use, further reducing its consistency as a default approach.
Overlaying these factors is a behavioural dimension. In high-pressure environments, clinicians tend to favour techniques that are reliable within their own practice and fit seamlessly into established workflows. For many, general anaesthesia offers a level of predictability and control that is easier to manage. While newer clinicians may be more comfortable with regional approaches, adoption still depends heavily on individual experience, training and confidence.
“Some of my anaesthesia colleagues have had training and are invested in regional, while others have less experience and will say “I need to use what I am comfortable with”, and will lean to general anaesthesia, when other options could also be used” – Thoracic Surgeon, NHS Northern Ireland
The result is a fundamental tension. Regional anaesthesia offers clear advantages in terms of recovery and patient outcomes, but general anaesthesia provides greater predictability and ease of standardisation. In practice, adoption reflects how this trade-off is managed within surgical teams, rather than a simple question of clinical superiority.
If regional anaesthesia is to become more widely embedded, the focus will need to extend beyond the technique itself to the way surgical care is organised.
In many settings, anaesthesia and surgery are still organised as sequential steps rather than an integrated process. Typically, a patient will first go to an anaesthetic room where a regional block is performed, and then there is a period of waiting for the anaesthetic to take full effect (10-15 minutes) before they are transferred into theatre for surgery. While this structure works, it introduces pauses into the pathway such as time where the operating theatre may be ready, but the patient is not, or vice versa. In high-throughput environments, these small inefficiencies can accumulate, making regional approaches feel slower and less practical compared to general anaesthesia, which can be initiated more predictably once the patient is in theatre. These pauses may amount to losing the possibility of operating on an additional 2-3 patients per surgeon per day. Emerging models are starting to rethink this separation by integrating anaesthesia more closely into the surgical workflow. Instead of treating it as a distinct step, select systems are trialling moving towards parallel processing, where preparation, anaesthesia, and surgical setup happen simultaneously across different patients. There is also growing exploration of performing certain nerve blocks within the operating theatre itself, reducing the need for separate spaces and transition times. Alongside this, efforts to streamline patient flow (from pre-operative preparation through to recovery) are helping to minimise delays and make timing more predictable. Together, these changes aim to reduce the operational friction that has historically limited the wider adoption of regional anaesthesia.
“Our main challenge with regional anaesthesia is the operational side. The lack of skilled staff and the time it takes to administer. Despite the reduced post-operational pain, hospital policy can mean we don’t use it enough” - Head of the Pain Unit, Department of Anaesthesiology, Germany
At the same time, there is an opportunity to rethink how solutions are designed and delivered. So far, much of the industry response has focused on product innovation, usually developing procedure-specific kits or bundled offerings that aim to simplify setup and support standardisation. While these can make individual steps more efficient, they often do not fundamentally change how regional anaesthesia is delivered in practice, and as a result, can feel interchangeable from one supplier to another. The broader challenge lies in the fact that regional anaesthesia is not just a product problem, but a pathway problem. Success depends on how well solutions fit into the realities of day-to-day clinical workflows, how easily they can be set up, how they interact with operating theatre timing, and how they support coordination between teams. This requires a deeper understanding of the full set of stakeholders involved, including not only anaesthetists, but also surgeons, theatre staff, and hospital management, each of whom experiences different parts of the process. In practice, however, engagement often remains limited to a narrower set of stakeholders, meaning that important perspectives are overlooked. As a result, companies risk missing critical insights into how regional anaesthesia is actually delivered on the ground. Without this broader understanding, even well-designed products may address only part of the challenge, leaving the underlying operational friction unchanged.
“Companies need to come in and spend time in the hospital, with different departments, and talk to staff besides the anaesthetists. All departments have a different approach. It is about understanding what each person in the chain is doing, and how their role is affected – the surgeons but also the theatre staff and the operating personnel. Gone are the days when a task is only for one – we are all involved in the same patient at the same time, and that needs to be understood” - Orthopaedic Surgeon, NHS England
Looking ahead, data-driven approaches may play a critical role in addressing some of the inherent limitations of regional anaesthesia. One of the key challenges today is variability: how long a block will last, how quickly it will take effect, and how a given patient will respond are not always predictable. This uncertainty makes it difficult to align anaesthesia precisely with surgical timelines and recovery pathways. Advances in data and analytics offer a way to reduce this unpredictability. By incorporating patient-specific factors such as age, anatomy, and comorbidities, alongside procedural variables and drug selection, it may become possible to better anticipate the duration and quality of a block before it is administered. In practice, this could mean selecting the optimal technique and drug combination to ensure that anaesthesia lasts exactly as long as needed (covering the procedure and early recovery period without unnecessarily delaying mobilisation). Over time, such capabilities could shift regional anaesthesia from a technique that requires a degree of estimation to one that is more precise and tailored. In doing so, it would address one of the key barriers to wider adoption: variability, and the uncertainty it introduces into otherwise tightly managed surgical workflows.
Regional anaesthesia is strongly aligned with the direction of modern healthcare. It supports faster recovery, reduces complications, and enables more efficient use of hospital resources. Yet its adoption remains uneven, shaped by the practical challenges of delivering it consistently across different settings.
The opportunity now is not to demonstrate its value, but to operationalise it. This will require progress not only in clinical techniques, but in training, workflow design, and stakeholder engagement. As these elements come together, regional anaesthesia has the potential to move beyond a high-performing option in selected cases to a more dependable standard of care, and one that supports both better patient outcomes and more efficient healthcare systems.
At Sector & Segment, we help you navigate the evolving regional anaesthesia landscape by identifying where clinical momentum is translating into real commercial opportunity. As regional techniques move from niche expertise to a driver of recovery-focused care, we support organisations in understanding where and how to play. Whether you are an established player in anaesthesia or entering the space through adjacent technologies, we help translate clinical trends into actionable growth strategies. Our team combines deep healthcare expertise with robust strategic capabilities to accelerate success through:
We collect, use, analyse and share data such as statistical or marketplace data and provide information such as opinions and insights for general information purposes only. The content of this article is not intended to amount to advice of any kind. No reliance should be placed on any statements made in this article, whether for medical, health, legal purposes or otherwise. Nothing in this article is an offer to enter into a binding contract or a recommendation, endorsement, guarantee or warranty of any kind. The content of this article is aimed at industry institutional professionals and is intended to serve as a concise initial reference and not as a complete reference source. You must obtain medical, professional or specialist advice before taking, or refraining from, any action on the basis of the content in this article.
You acknowledge that the content of this article may contain inaccuracies or errors and we expressly exclude liability for any such inaccuracies, incompleteness or errors to the fullest extent permitted by law. Neither we nor any third parties provide any warranty or guarantee as to the accuracy, timeliness, performance, completeness, or suitability of the information herein for any particular purpose. Some information may contain links to other sites, resources, or opinions of third parties and are provided for your information only. We have no control over the contents of those sites or resources and are not responsible for the content. In no event shall we be responsible for any loss or damage of whatever kind (including negligence) arising out of or in connection with your use of or reliance on any content within this article. You agree that your use of this content is at your own risk. This does not affect claims in respect of death or personal injury caused by our negligence and or excludes or limits liability that cannot be limited under law.
Healthcare Categories
Med Tech
Surgical Care
Therapeutic Areas



30 June 2025
Margarita Svarceva

6 June 2025
Maria Franco Hernandez

18 March 2025
Steven Yap
Strictly Necessary Cookies
These cookies allow the website to function properly, and it is not possible to use the website without them.
Statistical Cookies
These cookies allow statistical data to be collected about the use of our website.